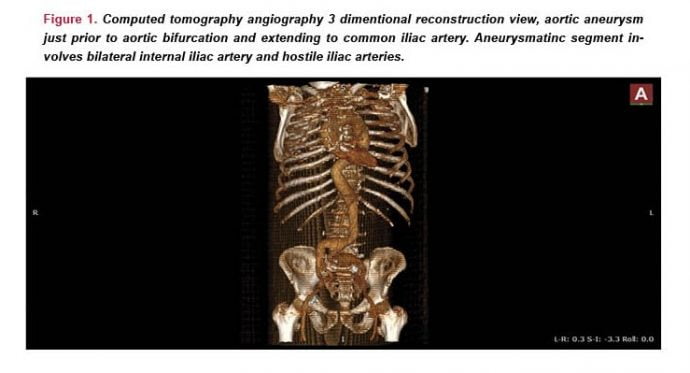
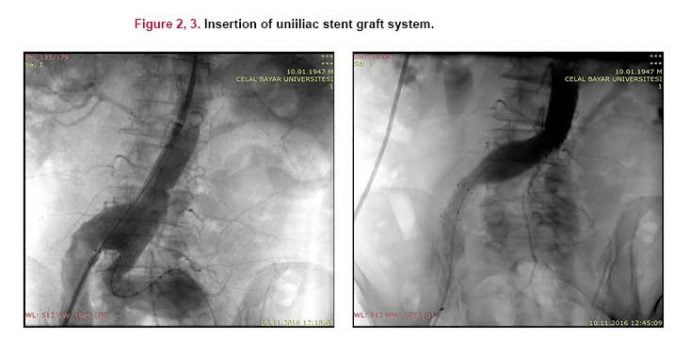
Hybrid treatment of aortic bifurcation aneurysm
The success of endovascular treatments mostly depends on anatomical suitability. Secure neck and iliac landing zones are required to avoid of endoleaks. Common iliac artery aneurysms frequently extend to the iliac bifurcation and complicates endovascular interventions. We report a hybrid operation of an abdominal bifurcation and extremely angulated iliac artery aneurysm that aneurysmatic segments involving both internal iliac arteries (IAA). We excluded the aneurysm by an uniiliac endovascular stent graft and contralateral IIA flow was supplied by retrograde filling from femoro-femoral bypass after ligation contralateral common iliac artery via retroperitoneal approach. It is important to consider alternative treatment modalities and in cases with extreme anatomic variations, to choose a hybrid endovascular approach may be the most feasible and less invasive.
Keywords: Endovascular treatments, hybrid operation, abdominal bifurcation, iliac artery aneurysm.
Full Text
Introduction
Infrarenal abdominal aortic aneurysm and iliac artery aneurysm are seen mostly together. The success of endovascular treatments mostly depends on anatomical suitability. Secure neck and iliac landing zones are required to avoid of endoleaks. Common iliac artery aneurysms (CIA) frequently extend to the iliac bifurcation and complicate the endovascular interventions. The preservation of circulation of at least one internal iliac artery (IIA) is highly recommended.
Case
Discussion
EVAR has become the firstline choice in abdominal aortic aneurysm repair. But there are some limitations to its use; hostile neck anatomy, hostile iliac anatomy (HIA) and aneurysmal enlargement involving bilateral internal iliac artery. Approximately 30% of patients treated by EVAR have ectatic or aneurysmal common iliac arteries not suitable for distal sealing zones. Bilateral internal iliac artery occlusion during endovascular repair may lead significant morbidity, including gluteal claudication, erectile dysfunction, ischemia of the sigmoid colon and perineum and spinal cord injury.(1,2,3)
In CIA aneurysms involving the IIA, there are some ways of preserving flow to IIA; Surgical revascularization of IIA via retroperitoneal or retroinguinal insicion. An uncovered stent can extend the sealing zones, whilst maintaining complete preservation of pelvic circulation and offers support to the covered stent-graft.(4) Iliac side-branched graft (IBG) or sandwich technique can maintain pelvic perfusion. However, these adjunctive procedures increase the risk of endoleaks and they need to be applied by an experienced interventionist because of its technical difficulties.(5-8)
The presence of narrow iliac arteries (diameter <7 mm), hemodynamic iliac stenosis or obstruction, severe or extensive calcifications (>50%iliac circumferential calcification), angulations (>90 degree), previous aortailiac/femoral graft was defined as HIA.(5) HIA or previous surgical or endovascular graft greatly limits the endograft’s maneuverability.(9)
This case have an aortic aneurysm just prior to aortic bifurcation and extending to CIA. The case is an example to hostile iliac artery because of severe iliac angulation and also it is complicated by aneurysmatic segment involving bilateral IIA ostium. The aneurysm is treated in combined fasion: endovascular and convential surgery. We used this approach for two reasons. First, to prevent recurrent king or stenosis of the left iliac endograft system due to extreme angulation to the right side. Secondly, to preserve the blood supply of at least one of the internal iliac artery. We think that it is important to consider alternative treatment modalities and in cases with extreme anatomic variations, to choose a hybrid endovascular approach may be the most feasible and less invasive.
Conclusion
Despite progress in endovascular therapy, large infrarenalble to use combined thoracic and abdomi-nal stent graft as an alternative treatment modality when the patient is not suitable for standard EVAR and open surgery.
References
- Faries PL, Morrissey N, Burks JA, Gravereaux E, Kerstein MD, Teodorescu VJ et al. Internal iliac artery revascularization as an adjunct to endovascular repair of aortoiliac aneurysms. J Vasc Surg 2001; 34(5): 892-9.
- Cochennec F, Marzelle J, Allaire E, Desgranges P, Becquemin JP. Open vs endovascular repair of abdominal aortic aneurysm involving the iliac bifurcation. J Vasc Surg 2010; 51(6): 1360-6.
- Bosanquet DC, Wilcox C, Whitehurst L, Cox A, Williams IM, Twine CP; British Society of Endovascular therapy (BSET). Systematic Review and Meta-analysis of the Effect of Internal Iliac Artery Exclusion for Patients Undergoing EVAR. Eur J Vasc Endovasc Surg 2017; 53(4): 534-548.
- Silingardi R, Tasselli S, Gennai S, Saitta G, Coppi G. Endovascular preservation of pelvic circulation with external iliac-to-internal iliac artery “cross-stenting” in patients with aorto-iliac aneurysms: a case report and literature review. J Cardiovasc Surg (Torino) 2012; 53(5): 651-5.
- Zeng Q, Huang L, Huang X, Peng M. Endovascular repair of abdominal aortic aneurysm with severely angulated neck and tortuous artery access: case report and literature review. BMC Surg 2015; 15: 20.
- Noel-Lamy M, Jaskolka J, Lindsay TF, Oreopoulos GD, Tan KT. Internal Iliac Aneurysm Repair Outcomes Using a Modification of the Iliac Branch Graft. Eur J Vasc Endovasc Surg 2015; 50(4): 474-9.
- Lim CS, Naji Y, Hussain ST, Pleban E, Wiszniewski A, Onida S et al. Modified Sandwich-graft Technique Employing Aorfix and Viabahn Stent-grafts to Preserve Hypogastric Flow in Cases of Complex Aortoiliac and Isolated Common Iliac Artery Aneurysms Including the Internal Iliac Artery Ostium. Eur J Vasc Endovasc Surg 2016; 51(3): 364-70.
- Donas KP, Torsello G, Pitoulias GA, Austermann M, Papadimitriou DK. Surgical versus endovascular repair by iliac branch device of aneurysms involving the iliac bifurcation. J Vasc Surg 2011; 53(5): 1223-9.
- Gallitto E, Gargiulo M, Faggioli G, Pini R, Mascoli C, Freyrie A et al. Impact of iliac artery anatomy on the outcome of fenestrated and branched endovascular aortic repair. J Vasc Surg. 2017; 6. pii: S0741-5214(17)31359-9. doi: 10.1016/j.jvs.2017.04.063. [Epub ahead of print] PubMed PMID: 28888759.